Sponsored Content
While social distancing is essential, “medical distancing”—staying away from the doctor’s office for fear of contracting COVID-19—is dangerous. Just as phrma.org’s latest campaign strives to remind people that seeking care is not only safe but necessary, we see it as our duty at PatientPoint to provide patients, physician practices, and brands the support they need to ensure effective engagements are still occurring at the point of care.

Our business is driven by a deep understanding of patient and physician behaviors and desires at critical touchpoints in the care journey. We know your business relies on these insights as well. That’s why we are continually talking to our network of physicians, analysts, and industry insiders to secure proprietary data that we can use to provide you with the most up-to-date insights into the pulse of marketplace.
Here are three new insights, according to patient-level claims data and the latest results of ongoing, independent COVID-19 patient surveys.
1. Patient visits are steadily increasing and now exceeding 2019.
While the impact on patient traffic was significant during the onset of COVID-19 in late March and April, since that time primary care office visits have steadily increased and returned to near normal ranges in June and July.
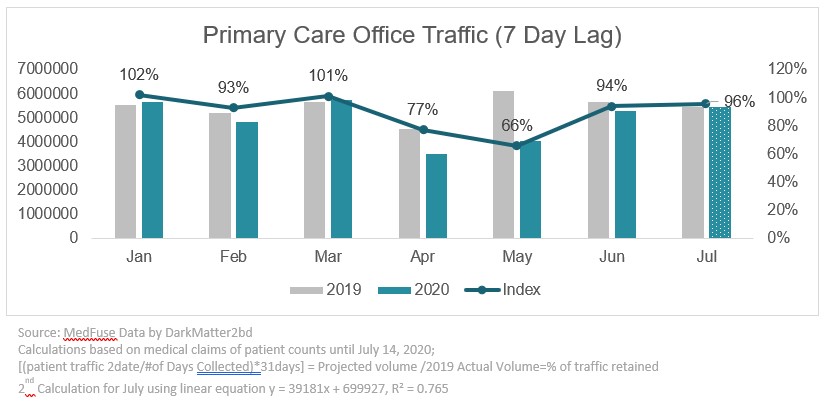
2. The second COVID surge is not impacting patient traffic in physician offices.
An additional look at trends across the country, using the same patient-level claims data, uncovers that primary care practices in most states have returned to their pre-COVID patient volumes (despite the second surge).
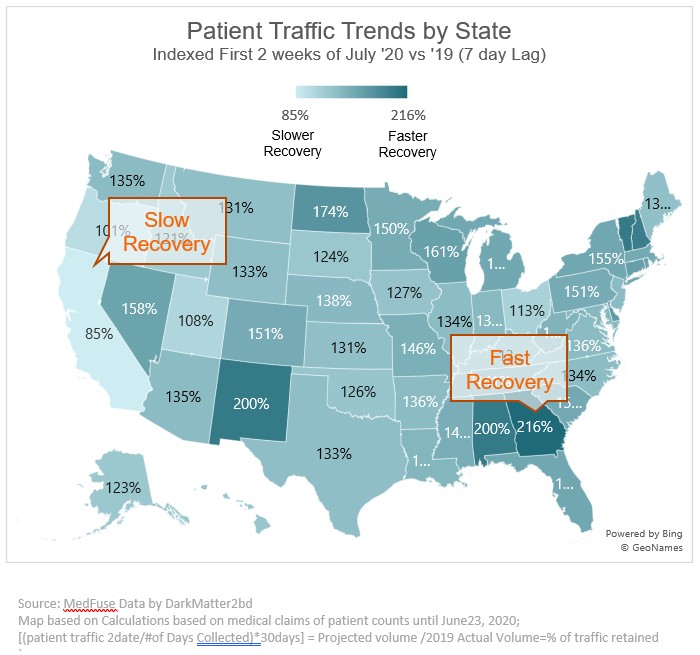
3. Telehealth visits are leveling off.
As more patients return to the doctor’s office, we see the percentage of telehealth visits now comprising approximately 10-11% of all primary care visits (compared to about 25% at the peak of COVID in mid-April). According to our recent consumer surveys, 72% of patients say they prefer in-person appointments.
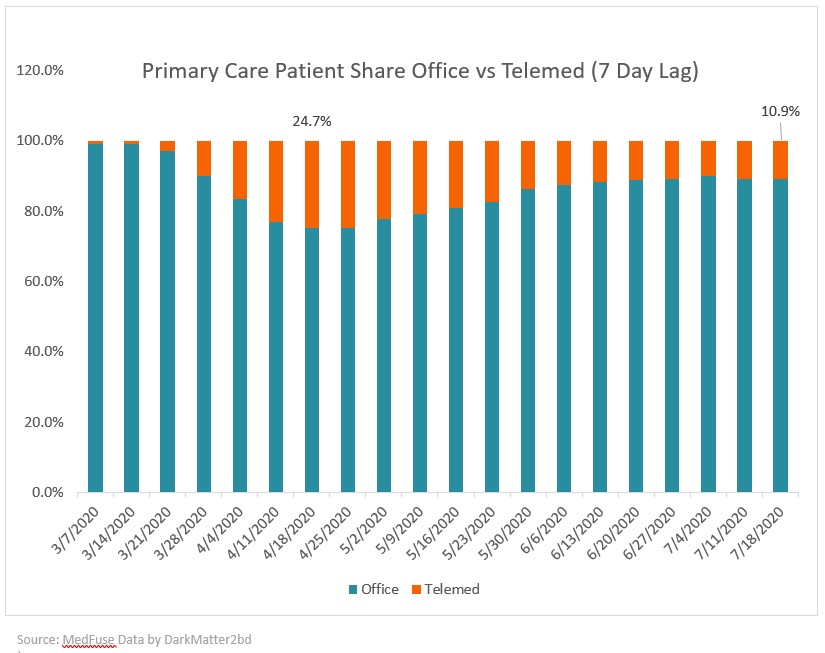
Through our ongoing data collection, we hope to separate fact from fiction about patient care and COVID-19, and provide an ongoing benchmark of real insights straight from doctors and patients during this unprecedented time. We will continue to apply what we’ve learned to ensure we make every doctor-patient engagement better at all points of care.
Keep up to date on all of our latest research and insights by visiting our COVID-19 News of the Day blog.


 One of my favorite things about PatientPoint is that we’re always finding innovative ways to improve patient engagement. Leading the charge on the technology side is David Guthrie, Chief Product Officer at PatientPoint and one of the most interesting and best hires we’ve ever had.
One of my favorite things about PatientPoint is that we’re always finding innovative ways to improve patient engagement. Leading the charge on the technology side is David Guthrie, Chief Product Officer at PatientPoint and one of the most interesting and best hires we’ve ever had. To help combat opioid addiction, PatientPoint® collaborated with Shatterproof – a nonprofit organization focused on ending the stigma of addiction and improving addiction treatment – to create a powerful opioid education program at the point of care. It launched nationwide in October 2017 across the digital PatientPoint engagement platform, reaching an estimated 15 million patients and caregivers each month in waiting rooms, exam rooms, and in the physician back office. The content is designed to increase the awareness of opioid addiction and encourage doctor-patient discussions about other treatment options.
To help combat opioid addiction, PatientPoint® collaborated with Shatterproof – a nonprofit organization focused on ending the stigma of addiction and improving addiction treatment – to create a powerful opioid education program at the point of care. It launched nationwide in October 2017 across the digital PatientPoint engagement platform, reaching an estimated 15 million patients and caregivers each month in waiting rooms, exam rooms, and in the physician back office. The content is designed to increase the awareness of opioid addiction and encourage doctor-patient discussions about other treatment options.
 I sat down with Charlie Greenberg, a respected healthcare industry veteran and an expert in point-of-care (POC) marketing, to discuss current trends in healthcare marketing. It’s a topic Charlie knows well, having worked for more than 30 years in the industry with giants like Saatchi & Saatchi, Wyeth, and Merck. Charlie currently serves as a media and marketing consultant, so he spends a great deal of time thinking about the ways brands can improve their reach and maximize their return on investment.
I sat down with Charlie Greenberg, a respected healthcare industry veteran and an expert in point-of-care (POC) marketing, to discuss current trends in healthcare marketing. It’s a topic Charlie knows well, having worked for more than 30 years in the industry with giants like Saatchi & Saatchi, Wyeth, and Merck. Charlie currently serves as a media and marketing consultant, so he spends a great deal of time thinking about the ways brands can improve their reach and maximize their return on investment. What’s the best pharma ad you see running on TV right now? I bet you could sing the jingle, but do you remember the specific brand? I’m the odd one that uses my DVR to skip TO the commercials – but you and I are not the average healthcare consumers. That’s why, despite the strength of TV, when it comes to messaging to patients, you have to pull that message through when they are going to be most receptive – in the doctor’s office.
What’s the best pharma ad you see running on TV right now? I bet you could sing the jingle, but do you remember the specific brand? I’m the odd one that uses my DVR to skip TO the commercials – but you and I are not the average healthcare consumers. That’s why, despite the strength of TV, when it comes to messaging to patients, you have to pull that message through when they are going to be most receptive – in the doctor’s office.
 The results demonstrate that patient engagement solutions at the point-of-care can provide pharma with an opportunity to drive better physician-patient discussions, insert their brand into those discussions and ultimately help educate on better treatment decisions. This is an unprecedented and unique ability to impact both audiences at that magic moment when treatment decisions are being made.
The results demonstrate that patient engagement solutions at the point-of-care can provide pharma with an opportunity to drive better physician-patient discussions, insert their brand into those discussions and ultimately help educate on better treatment decisions. This is an unprecedented and unique ability to impact both audiences at that magic moment when treatment decisions are being made. What are the challenges you see in planning for point of care? One that I see has risen is the need for a common currency: Is it doctors? Locations? Impressions? It’s critical to compare apples to apples when putting that buy in a spreadsheet, as practices are definitely not created equal.
What are the challenges you see in planning for point of care? One that I see has risen is the need for a common currency: Is it doctors? Locations? Impressions? It’s critical to compare apples to apples when putting that buy in a spreadsheet, as practices are definitely not created equal. The theme of this month’s newsletter is consumer trends. Here’s a recent one worth talking about: According to
The theme of this month’s newsletter is consumer trends. Here’s a recent one worth talking about: According to